Improved cardiac diagnostics, physician collaboration and awareness of congenital heart conditions in adults led to the diagnosis of a complex congenital heart defect followed by a minimally invasive repair that has a 69-year-old woman breathing easier. The unique team is all under one roof at Sarver Heart Center and Banner – UMC Tucson.
Looking back, Patricia Fickett, a native of San Simon, Ariz., has experienced symptoms of her congenital heart condition for much of her life. She always was told she had a heart murmur, but that it was nothing to worry about. At age 3, she was diagnosed with anemia, but seemed to outgrow it. As a student in a small-town high school where everyone participated in sports so the school could have a team, she was known as the person who consistently could not run distances without “running out of air.” She described her heart palpitations as butterflies that would sometimes feel like hummingbirds.
Seen by a cardiologist after she had a bout with rheumatic fever around age 20, Mrs. Fickett was told she was doing well, considering her heart condition that was described only as a “heart murmur.” “Again, the doctor said don’t worry unless I started having problems,” said Mrs. Fickett. She went on to have successful pregnancies and didn’t pay much attention to her heart condition, until she was in her fifties and doctors became concerned about her enlarged heart.

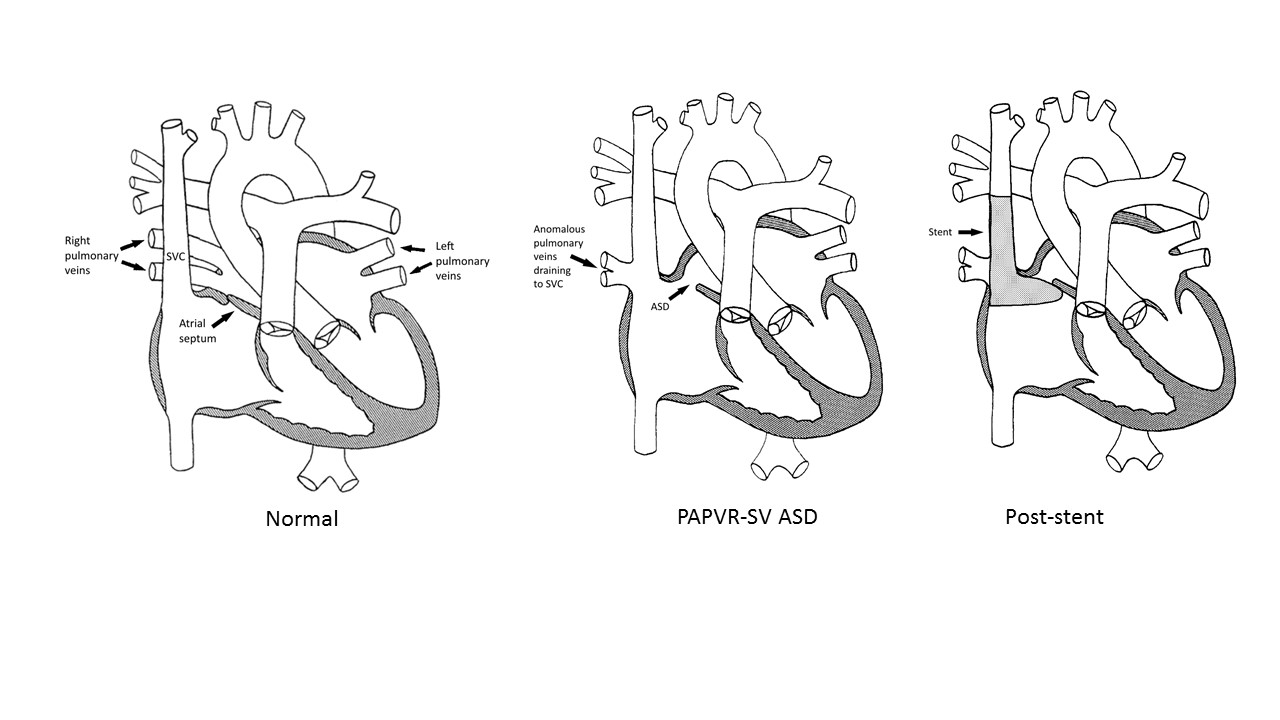
Dr. Janardhanan performed a 3D-transesophageal echocardiogram (3D-TEE), cardiac MRI and CT scan of the chest. The 3D reconstructions from the advanced cardiac imaging confirmed that Mrs. Fickett had a moderately complex congenital heart defect. She had partial anomalous pulmonary venous return (PAPVR), where some of the veins that bring oxygen-rich blood from the lungs back to the heart do not return to the normal location. In Mrs. Fickett’s case, as in most patients with PAPVR, this was accompanied by an atrial septal defect (ASD). This combination of defects leads to excessive amounts of blood flow to the lungs and are a rare cause of pulmonary arterial hypertension, but may cause only relatively mild symptoms through much of a patient’s life.
Dr. Janardhanan, professor of medicine and medical imaging at UA College of Medicine – Tucson, consulted Michael Seckeler, MD, MSc, an interventional pediatric and adult congenital cardiologist who specializes in repairing congenital heart defects through minimally invasive catheter procedures, and Franz Rischard, DO, a specialist in pulmonary hypertension. Drs. Rischard, associate professor of medicine, and Seckeler, associate professor of pediatrics, collaborated on a diagnostic catheterization procedure to measure the pressure and blood flow in Mrs. Fickett’s heart and lungs. “Mrs. Fickett had four times the normal amount of blood going through her lungs because of her congenital heart disease and this was the cause of her symptoms,” said Dr. Rischard.
While these congenital heart defects typically are repaired with open-heart surgery using heart-lung bypass, the Banner – University Medical Center Tucson Congenital Heart team was unsure that this would provide the best outcome for Mrs. Fickett because of the stress on her body, so less invasive options were considered.
Her anatomy was quite complicated, so Dr. Seckeler created and printed a 3-D model of Mrs. Fickett’s heart from the CT scan raw data, using a 3-D printer obtained through a 2015 Sarver Heart Center Investigator Award. With the model in hand, Dr. Seckeler was able to plan a minimally invasive, catheter-based procedure previously performed only a handful of times around the world, avoiding open-heart surgery. He also was able to use the model to explain the congenital heart defect and proposed intervention to Mrs. Fickett and her husband, Chuck Fickett.
In the cath lab, Dr. Seckeler placed a large covered stent in Mrs. Fickett’s superior vena cava (upper body vein) and created the wall that had never formed between the left and right heart. As soon as the stent was placed, her lung blood flow was down to almost the normal amount and her lung pressures returned toward normal.
“A week later, I made a meal for one of our church families who had suffered a loss. I now have more energy and no more fatigue. I’m active in my church and I returned to substitute teaching,” said Mrs. Fickett. “God took care of me for 69 years and decided I needed to be fixed, so He sent me to my miracle workers. There is no word adequate to express my gratitude to this gifted group of doctors, except, ‘Thank you.’”
“Having a team of specialists in Tucson able to diagnose and treat patients with complex congenital heart defects is a great asset. The UA Sarver Heart Center and Banner – University Medical Center Tucson have the longest standing and most experienced team to help patients in Tucson and from all over Arizona,” said Dr. Seckeler.
“While most adult congenital heart patients have undergone some type of heart surgery in childhood, at least 10 percent are not accurately diagnosed until adulthood. Mrs. Fickett’s cardiologist had suspicions about an underlying cause and referred her to Dr. Janardhanan who applied advanced diagnostic imaging, along with an awareness and direct access to the congenital heart specialists and cardiovascular scientists located under the same roof at BUMC-T/Sarver Heart Center. This permitted a team approach that resulted in the innovative, minimally invasive trans-catheter heart repair for Mrs. Fickett’s congenital heart defect. This multi-disciplinary congenital heart environment is unique in Arizona and provides a tremendous resource for adults living with congenital heart disease,” said Scott Klewer, MD, professor of pediatrics and medicine at UA College of Medicine – Tucson and the Sarver Heart Center’s Peggy M. Barrett Endowed Chair for Congenital Heart Disease in Adults.