Researchers at the University of Arizona College of Medicine - Tucson have launched a Phase II clinical study to assess the long-term effectiveness of “inspiratory muscle training” for reducing blood pressure and improving cardiovascular health in adults with obstructive sleep apnea.
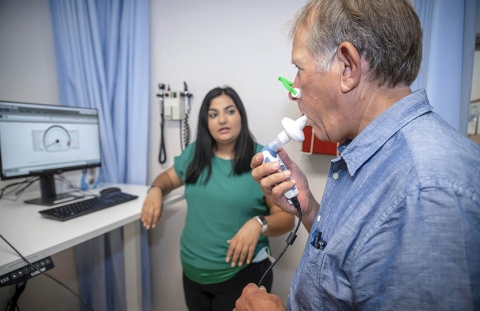
E. Fiona Bailey, PhD, professor of physiology at the UArizona College of Medicine – Tucson, was awarded a five-year, $3.4 million grant from the National Institute on Aging, a division of the National Institutes of Health, to build on her group’s previous research that showed a respiratory workout entailing 30 breaths a day can lower blood pressure.

Obstructive sleep apnea is a serious health condition in which the muscles of the throat relax during sleep and collapse inward so that air cannot reach the lungs for a short period. This causes oxygen deprivation and repeated awakening from sleep. Together, nightly oxygen deprivation and the inability to achieve uninterrupted sleep contribute to an increased risk of developing high blood pressure and cardiovascular disease. Obstructive sleep apnea affects about 50% of adults in the U.S. and nearly 1 billion people worldwide.
Results of early studies by Dr. Bailey’s group showed inspiratory muscle training builds respiratory muscle strength and has a surprising secondary benefit – it lowers blood pressure. The reduction in blood pressure is greater than that gained from traditional aerobic exercise and in many instances, can exceed reductions achieved with blood pressure medications.
In the current clinical trial, Dr. Bailey and her research team will implement inspiratory muscle training over six months in a larger group of 50-to-80-year-old adults with obstructive sleep apnea and above-normal blood pressure. The team will follow up with participants three months after the training ends to see how long the blood pressure-lowering effects last. Joseph Alpert, MD, professor of medicine in the Division of Cardiology, and Saif Mashaqi, MD, associate professor of medicine in the Division of Pulmonary, Allergy, Critical Care and Sleep Medicine, are clinical physicians on the study. The team also includes collaborators at the University of Colorado at Boulder.
Study participants will undergo initial screenings of cardiovascular, respiratory and sleep health. Eligible participants will be randomly assigned to one of two training groups, one emphasizing high resistance training the other emphasizing low resistance training. Participants in both groups will perform their training at home and complete 30 breaths per day, 5 days a week, for 24 weeks.
Inspiratory muscle training originally was devised for use by athletes and people with breathing problems, such as chronic obstructive pulmonary disease, asthma and bronchitis. Dr. Bailey has adapted the protocol for everyday use by adults with obstructive sleep apnea. In its current format, inspiratory muscle training can be performed at home, at work or when travelling, using a hand-held training device similar to an inhaler.
Continuous positive airway pressure, or CPAP, is the standard therapy for obstructive sleep apnea and is effective at reducing oxygen deprivation during sleep, but many users discover they are unable to tolerate it throughout the night.
Regular aerobic exercise can help and is important for cardiovascular health, but current recommendations are for 150 minutes per week of moderate intensity exercise. This amount of exercise can be a difficult to achieve – fewer than 30% of American adults meet this minimum – and may be especially challenging for adults with obstructive sleep apnea, many of whom experience chronic fatigue and excess daytime sleepiness.
“New cost-effective and time-efficient strategies are needed to manage the health issues caused by obstructive sleep apnea,” said Dr. Bailey, also a member of the BIO5 Institute. “It is vitally important that we devise new approaches to help people keep their blood pressure under control and improve cardiovascular health.”
Dr. Bailey’s research has roots in Sarver Heart Center’s Investigator Awards program. In 2014, she mentored Jennifer Vranish, then a graduate student (now a PhD), who was awarded $25,000 for her project, “Respiratory Training and Cardiovascular Health in Sleep Apneics.” This project supported Vranish’s research during her doctoral dissertation and led to subsequent national funding.
“Sarver Heart Center’s support was key in getting Jennifer’s idea off the ground and the outcome provided us preliminary data for an American Heart Association Grant in Aid which in turn provided us the preliminary data for our current RO1 from NIH/National Institute of Aging,” said Dr. Bailey.
Clinical Trial Information
For more information on participating in the clinical trial, contact Lupita Ramos-Barrera at 520-626-0836 or baileylaboratory@email.arizona.edu, or visit https://redcap.link/breathe
Research discussed in this publication is supported by the National Institute of Aging, a unit of the National Institutes of Health (R01AG065346-01A1). This project is approved by the University of Arizona Institutional Review Board.
Your Support Has Big Impact
Sarver Heart Center's education of future cardiologists, advancement of patient care through science and clinical trials, and long-standing commitment to community outreach and education, are made possible because of support from readers - like you. Please consider a donation to support our mission as we work to innovate life-saving patient care.
Yes, Try This at Home!
If you're not eligible or able to participate in this clinical trial, you can try breathing resistance exercises on your own using any variety of devices available online. Dr. Bailey said devices come in a wide range of styles and prices, all can be effective. If you would like to learn these breathing exercises, please email Dr. Bailey at ebailey@email.arizona.edu. She is willing to teach groups remotely via Zoom.

